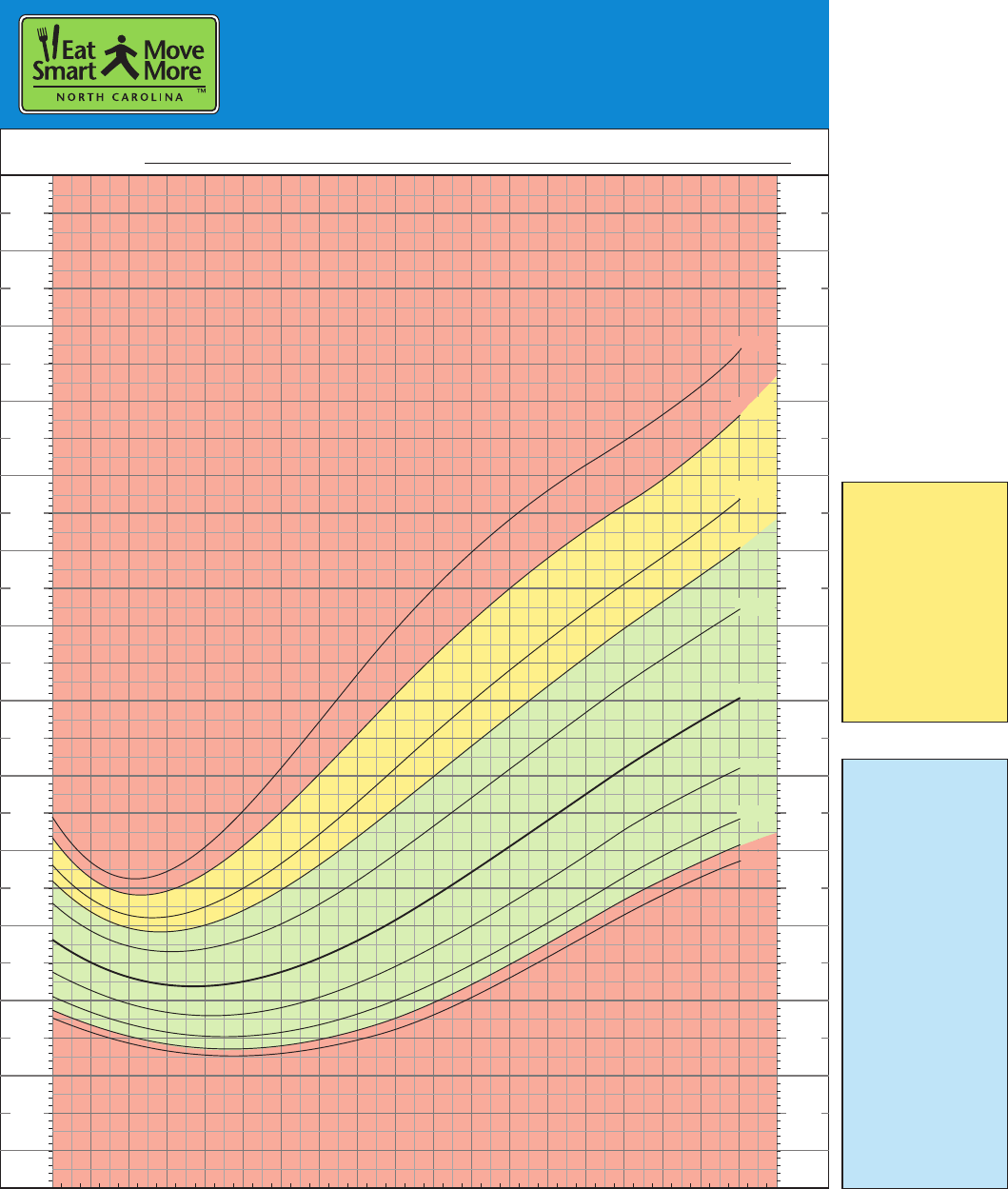
This study examines the BMI z-score of children within the wider Bristol area as they progress from Year 1 (aged 5–6 years) to Year 4 (aged 8–9 years) of primary school. This might prove a cost-effective approach to tackling childhood obesity by precluding the need for weight measurements or engagement of an already overweight child in an intervention and the associated challenges that this brings, whilst also providing overweight and obesity prevention in normal weight children. This is important as it may provide justification for the development of parent-only interventions to prevent parental weight gain, with the indirect effect of preventing child weight gain. Many studies have demonstrated that parental weight loss during these programmes is correlated to a reduction in child BMI z-score More recently, evidence is emerging that children do not need to be in attendance at an intervention for their weight to improve and parent-only interventions (with the main aim of addressing the child’s overweight status) may be a more cost-effective method Fewer studies simply observe the impact of change in parent BMI over time (gain or loss) on a child’s BMI z-score when no intervention is provided. The influence of parents on a child’s weight underpins the theoretical basis of family-based obesity interventions (where both the child and parent attend the intervention), which are viewed as an important strategy for the treatment of childhood overweight and obesity. Parental obesity is a known risk factor for childhood obesity though the literature is less clear whether there are differences in associations in weight according to parental gender and child gender. Overweight children are more likely to become overweight adults, with the associated socioeconomic and health related consequences presenting a major public health challenge. Within the 34 Organisation for Economic Cooperation and Development (OECD) countries, the UK is ranked 9th for childhood overweight prevalence In England, the National Child Measurement Programme (NCMP) assesses weight status in Reception (aged 4–5 years) and Year 6 (aged 10–11 years) of primary school and local analyses have shown a rise in child BMI z-score between these ages. The global prevalence of overweight and obese children has risen in the past four decades from 4% in 1975 to 18% in 2016. Further studies are needed to explore the impact of parental weight change on child BMI z-score and whether interventions targeted at overweight or obese parents, can improve their child’s BMI z-score. The key indicator of higher child BMI at Year 4 is high BMI at Year 1. 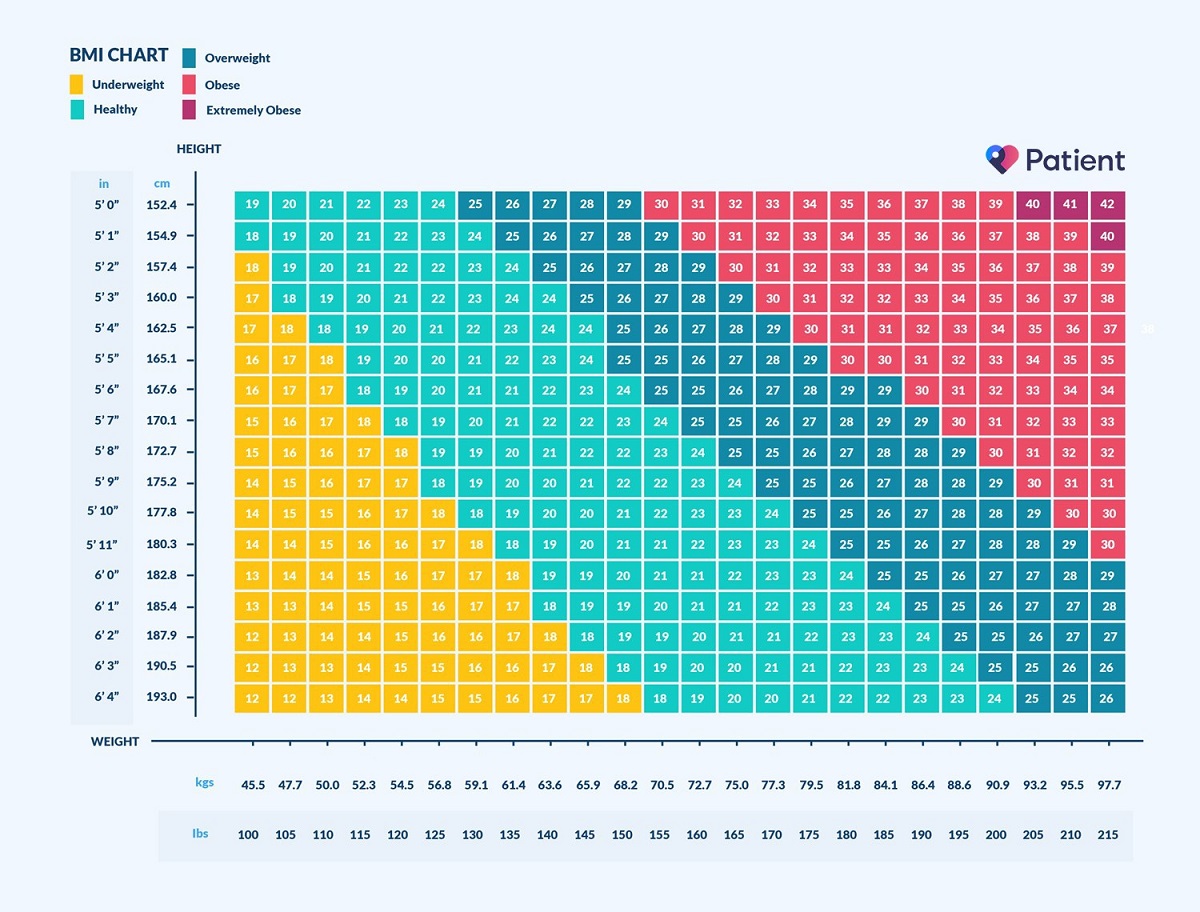
Parental BMI change was not significantly associated with Year 4 child BMI z-score. For every unit increase in parent BMI, there was an increase in child BMI z-score of 0.047 in Year 1 ( p = < 0.005) and of 0.059 in Year 4 ( p = < 0.005). Child mean BMI z-score score increased from 0.198 to 0.330 ( p = < 0.005) between these timepoints. There was a strong association between child BMI z-score at Year 1 and 4. The influence of change in parental BMI between Year 1 and Year 4 on child BMI z-score in Year 4 was explored through regression analyses, adjusted for baseline BMI z-score. Multivariable linear regression models examined the cross-sectional associations between child BMI z-score and parent BMI in Year 1 and 4. 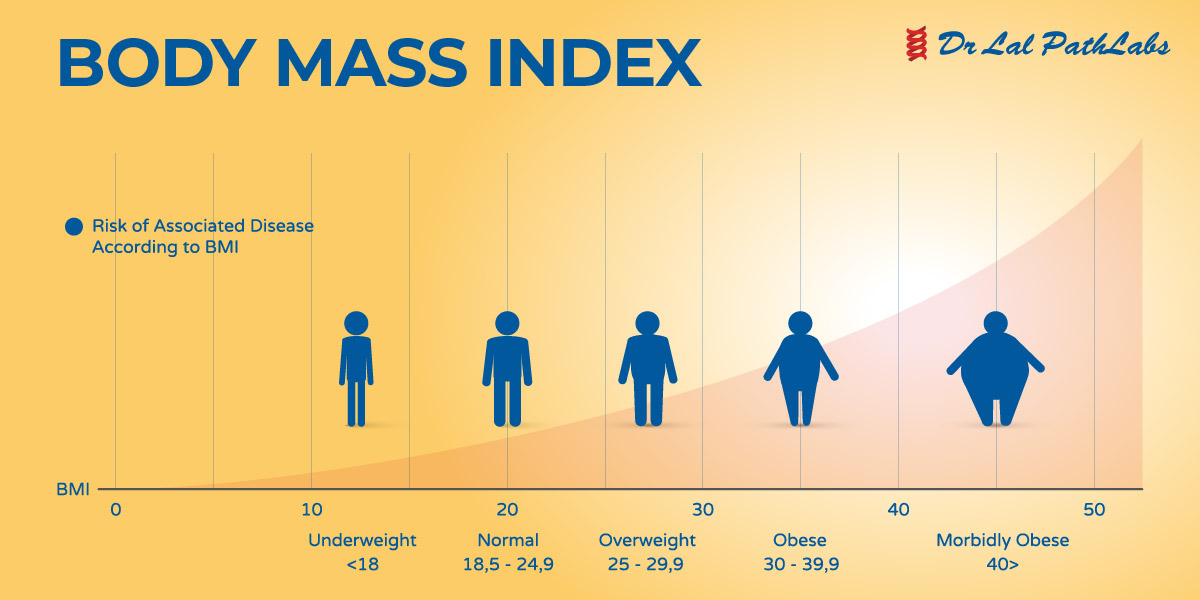
A paired sample t-test examined changes in child BMI z-score between Year 1 and 4. Methodsĭata from the longitudinal B-ProAct1v study (1837 participants) were analysed. This is important to understand for the development of effective obesity interventions. This paper aims to explore change in BMI z-score through childhood and the association between parent BMI and child BMI z-score.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
